Are you suffering from diarrhea, constipation or both?
Looking for a health practitioner who not only understands IBS (irritable bowels), but has recovered from it personally?
Look no further! This page is full of information on IBS. Dr. Karin personally suffered with IBS, and she shares her wealth of information on IBS in her book, "Combat Irritable Bowels":
Dr. Karin also does weekly facebook lives to share her wealth of information. For your connivence, we put all the videos on Irritable Bowels here on this page:
This Facebook Live shows how to massage your constipation away: https://www.facebook.com/Drumm...
For more tips for constipation
Why see a chiropractor for GERD or
Irritable Bowel Syndrome?
Better communication between the brain and body makes for better functioning organs, leading to a healthier body in general. I love chiropractic because chiropractic works, not only for back and neck pain, but for general wellness. Chiropractic adjustments restore mobility and space to the spine, and chiropractors educate their patients on healthy lifestyle habits to reduce the cause of their symptoms, even symptoms of GERD and Irritable Bowels.
Chiropractors are primary-care physicians who complete just as many years of education as an allopathic medical doctor. Chiropractors are more than just neck and back doctors who manipulate (adjust) spines. A medical doctor’s education is filled with pharmacology because their primary form of treatment is prescribing medications. This approach often just removes or glosses over symptoms instead of dealing with the underlying causes.
However, chiropractors can help you with your IBS naturally, through supplements, dietary modifications, adjustments and more. Chiropractors can determine if more invasive treatments are needed and will refer you to a specialist accordingly.
The health benefits of an adjustment are often more than patients expect because the chiropractor is moving the vertebrae of the spine apart and creating more space for the nerves that exit the spinal cord. Nerves don’t like pressure; they function better with space. When nerves experience less pressure, they are more efficient at sending signals between the brain and the muscles and organs, making for overall improved health.
Nerves that exit the mid-back region send signals to the organs in the mid-torso, including the lungs, stomach, spleen, and liver. After treating for mid-back pain, I have heard things like “My GERD has improved”, "I can eat foods that normally triggered my IBS", even reports like “My asthma is better.”
Nerves that exit the lower back region of the spine send signals to the organs in the lower torso, including the lower intestines, reproductive organs, and lower extremities. After treating lower back pain, I often hear things like “My bowel movements have been more regular than ever,” “My menstrual cycle is more normal, and my cramps are less painful,” “My ED seems to have resolved,” and “I thought I was infertile, and now I am pregnant!”
To learn how and why chiropractic treatments help more than just low back pain, CLICK HERE.
You don't have suffer with IBS. Why wait?
so we can individualize a treatment for your specific needs.
See how the chiropractic lifestyle can change your life!!!
Watch our Facebook Live to learn about colostrum and how it can help your Irritable Bowels: https://www.facebook.com/Drumm...
Recipe that helps with Irritable bowels, IBS-C, IBS-D and IBS-M
WANT TO LEARN ABOUT SUPPLEMENTS THAT CAN HELP?
EXCERPTS FROM DR. KARIN'S BOOK,
"Combat Irritable Bowels":

CHAPTER 1: Dr. Karin Drummond's Personal Story With IBS:
I WAS A HEALTHY KID who had the normal periodic earaches and sore throats. My mom was the perfect mom who stayed home and cared for us kids. So, of course, every time I had the sniffles, she took me to the medical doctor.
This was during the late 1970s and early ’80s. Back then, doctors liberally prescribed antibiotics. Everyone was happy:
· Mom was happy she got something to help her ailing little girl.
· I was happy because I was verifiably sick and got to take yummy, sweet-tasting medicine.
· The doctor was happy he could help.
So, for the first decade of my life, I was prescribed antibiotics several times a year!
Otherwise, I was a happy, healthy little thing. I played on the beaches and in the forests of the rural coastline of British Columbia, Canada. We lived in Tofino, a small fishing village at the end of the Trans-Canada Highway. Despite my village’s tiny size, we did have a candy store, which I frequented often.
Unbeknownst to me, my love of sweets combined with several days’ worth of antibiotics several times a year created the perfect condition for irritable bowel syndrome (IBS) in my belly.
Why Would Sweets and Antibiotics Lead to Irritable Bowels?
Antibiotics kill bacteria. This sounds good, right? Unfortunately, besides killing the bad bacteria, antibiotics also kill the much needed probiotics (the good bugs) in our colon (Figure below).
Figure 1‑1: Antibiotics kill the good and the bad bacteria.
We have an Amazon jungle in our lower intestines. In the last decade, sciences has started to learn how import this flora is to our general good health. These bugs don’t just help us digest our food; they also help regulate our bowel movements and support our immune systems.
If this good flora gets slaughtered by antibiotics, our guts become void of the living organisms that protect the lining of our intestines from opportunistic bugs.
Without probiotics, our colons become a breeding ground for whatever nasty bacteria find its way to our colon. Like a petri dish, the colon is a perfect environment for bugs to grow, especially if it’s full of sweets (carbohydrates) for them to feed on. If the bad bacteria replenish before the good bugs do (which is what happens in a sugary environment), the bad bugs will take over. This, quite literally, results in a nasty mess.
With repeated usage of antibiotics “clear cutting” the “Amazon” in my belly, my good flora was so depleted that normally harmless bacteria took over, flourishing in the sweet environment, resulting in their waste products poisoning my body.
You don't have suffer with IBS. Why wait?
Constant Diarrhea Leads to Other Health Issues
I was only eleven years old when my bowels went haywire. It started with frequent diarrhea. My mom got concerned when I reported painful diarrhea. She took me to our medical doctor, and he requested samples.
That was embarrassing.
The labs failed to show any cause—no parasites, no blood, no laxatives (yes, they checked to make sure I wasn’t anorexic).
Because the doctors failed to find a disease, they decided nothing was wrong with me and my diarrhea should simply clear up on its own.
It didn’t. It got worse. Sorry for the gory details, but anything I ate went right through me. My bowels were so inflamed that I was literally pooping out what looked like snotty phlegm surrounding food particles.
I repeatedly went to the medical doctor that year because I continued to suffer from mucousy diarrhea. I was loosing weight and getting weak. I also stopped growing.
At the clinics and hospitals, I was poked and prodded with needles and scopes as the doctors tried to determine the cause of my diarrhea.
They were very thorough in their testing. They put me through a colonoscopy, looking for evidence of Crohn’s disease or ulcerative colitis.
Eureka, You Have IBS!
When all tests were negative, the medical doctors finally came to a conclusion. I must have irritable bowel syndrome, a newly discovered condition that was not very well understood.
Since then, I have learned that IBS was not so new. Osler coined the term Mucous colitis in 1892 (almost one hundred years before my diagnosis). It was just such a rare condition that most doctors had not heard of it.
Then, since the introduction of antibiotics, terms like spastic colon, unstable colon, mucous colitis, and colonic neurosis along with IBS started popping up in research literature. This was because people with IBS were, and continue to be, on the rise. What was once a rare condition is now very common as one in five Americans suffer with some form of IBS![1]
IBS has been on the rise in America since 1945 (the era of the antibiotic). I believe this is more than just a coincidence of time. IBS is also on the rise in other developing countries, despite an increase in hygiene (or because of it).[2]
I now believe that I had pseudomembranous colitis, a condition in which the lining of the intestines becomes so inflamed and full of mucous that the body increases the bowel movement frequency to expel it, negatively affecting the absorption of nutrients.
At my worst, I weighed only 85 pounds (30 pounds underweight) and was too weak to brush my own hair or stand up from a squatting position. I had had enough. I begged my mom to sign the papers to release me from the hospital. I swore I would die if she didn’t.
Against her better judgment, she did as I asked, allowing me to escape the clutches of the failing medical paradigm.
I can’t image how hard it was for her to sign the paperwork stating that she was going against the doctor’s orders and that I, her baby girl, was at risk of dying if she took me away from their care.
Remember, this was before the Internet was readily available. This was before chiropractic education was what it is today. Luckily, I had a grandmother who was knowledgeable in herbal remedies and an uncle who was studying to become a chiropractor.
They both advised me to eat more vegetables (despite the medical doctor telling me not to eat fiber because my diarrhea was so bad), yogurt (despite the medical doctor warning me about the hazards of dairy products because they are “mucous forming” and I may be lactose intolerant), and herbs (despite the medical doctor warning me that herbs were not safe to take in my condition).
Basically, my medical doctors were wrong.
I needed to feed my good flora with vegetables (Figure 1-2); replenish the good bugs like those found in yogurt (acidophilus); and gently clean out the bad bugs without harming the good bugs (with the help of herbs).
Figure 1‑2: Replenishing and feeding the good bacteria for good health.
Within months, I was gaining weight, strength, and good health. Interestingly, all the medical doctors I worked with, after hearing my story, told me that I finally just got over it.
I’m not saying that is not a possibility; maybe it was a simple coincidence of time. But to me, a true doctor should learn from their patient’s anecdotal evidence; they should explore it to see if there was a causal relationship to their home remedy and the resolve of their condition.
It could be coincidental that I finally got well when I changed my diet and took herbal remedies. My point is, if someone gets better after a change in diet, exercise, sleep pattern—anything—I believe it is worth exploring, no matter how ridiculous and unbelievable the home remedy may seem.
IBS - Why I Am a Chiropractor
This experience made me promise myself that I was going to be a true doctor, one who listens to her patients, constantly learns from and for them, does no harm first, and finds a way to help the body heal itself.
That is why I am a chiropractor today.
I wanted to learn how to help the body heal itself versus just prescribing a drug to minimize symptoms of a dis-ease. I am grateful for medical doctors because they shine in medical emergencies like appendicitis (not something I can adjust away or you can heal with diet and exercise). Where the medical profession is lacking is in wellness and prevention. This is where chiropractic shines.
You don't have suffer with IBS.
Why wait?
to schedule an appointment.
Now, I am going a step further. I am writing books so I can assist those beyond my hometown and help them determine the cause of their symptoms, what to do about it, and whom to turn to for help.
Don't assume it is Irritable bowel syndrome -
confirm with a healthcare provider
Rule out more serious conditions
BEFORE I REVEAL how to cure your irritable bowel symptoms; first I must inform you when it is imperative to seek medical attention. It would be irresponsible of me to say you could self-treat what appears to be IBS when your symptoms are actually the result of a different underlying disease that needs medical treatment, if not immediate care.
Seek immediate medical attention if you have any of these symptoms:
· Blood in the stool (the blood may be from a hemorrhoid if bright red, but it could also be a sign of bleeding ulcers or cancer). If the bleeding is occurring higher up in the GI tract, it will appear dark (almost black like coffee grounds).
· Sharp abdominal pain that increases over time (could be appendicitis)
· Unexplained weight loss (a sign of cancer)
· Unexplainable night sweats (may be hormonal imbalances, but this is also a sign of cancer)
· Mucous in the stool (a sign of inflammation and/or infection)
· Your symptoms are increasing in frequency, intensity, or duration. If you experience this, seek immediate medical attention! It could be a sign of a more serious condition.
What conditions your IBS may be a result of:
IRRITABLE BOWEL SYNDROME (IBS) is a condition in which patients experience abdominal pain, bloating, and a change in bowel movements. It can lead to malnutrition (weight loss, anemia, and wasting of muscle). Or you may experience weight gain; as your body searches for the nutrients it needs, your appetite may increase, and your caloric intake exceeds you daily need. IBS can also cause other problems like joint pain and muscle pain. You may also develop leaky gut syndrome; this occurs when the lining of the GI tract inflames to the point that toxic substances leak into your bloodstream from the fecal material.
Irritable Bowel Syndrome (IBS) is broken down into four types:[1]
· IBS-C: Frequent constipation
· IBS-D: Frequent diarrhea
· IBS-A: Alternating between types C and D
· IBS-M: Mixed diarrhea and constipation
With increased movement of the bowels (diarrhea), the digestive juices from the stomach and duodenum (the section of your small intestine right below your stomach) can flush lower down the digestive tract. The lining can’t handle the digestive juices, causing them to ulcer.
With decreased movement of the bowels (constipation), the colon can become so enlarged with the impaction of fecal matter that surgeons may feel the need to remove the colon, which results in the patient using a colostomy bag.
Once a rare condition, IBS is now the most common chronic inflammatory condition after rheumatoid arthritis! Millions of patients see a doctor for IBS, while many more people suffer from the condition but don’t get treatment.[2]
Personally, I believe that IBS is a “garbage can diagnosis”—a diagnosis that uses fancy words to describe the symptoms the patient is suffering from without understanding why or what to do about the root cause. Such garbage can diagnoses result in treatments that just manage the symptoms, which is detrimental to one’s long-term health.
DIAGNOSING Irritable Bowel Syndrome SHOULD BE A LAST RESORT
MY BIGGEST PET PEEVE is when a patient comes to me with what I call a “garbage can diagnosis.” The patient tells me she’s been “diagnosed” with a condition that uses big Latin words. The terms describe the patient’s complaints without providing a true understanding of the cause. Often, the diagnosis of IBS is given when every known differential diagnosis (other conditions that share similar symptoms) is ruled out.[1]
Basically, when you are diagnosed with Irritable Bowel Syndrome, the doctor is telling you that you have irritated bowels, and they don’t know why.
The intent of this chapter is to help you verify that your healthcare providers have looked at all of these possible conditions before diagnosing you with Irritable Bowel Syndrome.
[1] Spiegel, et al., “Is Irritable Bowel Syndrome a Diagnosis of Exclusion?" A survey of primary care providers, gastroenterologists, and IBS experts,” American Journal of Gastroenterology.
Ruling Out Medical Conditions that mimic ibs
Many diseases mimic the symptoms of IBS (abdominal pain, bloating, and a change in bowel movements). It may appear you have IBS, but your symptoms may be the result of a disease. Before concluding that you have IBS, your doctor should be able to rule out:
· Crohn’s disease
· Gall bladder dysfunction
· GERD (gastroesophageal reflux disease)
· Infectious colitis
· Lymphocytic colitis
· Parasites
· Pseudomembranous colitis
· Ulcerative colitis (ulcers in your colon)
· Other medical conditions of the GI (gastrointestinal) tract
· Side effects from medications that could irritate your bowels, irritate the lining of the stomach, and/or cause constipation
In addition to all of those disorders, you have to make sure your bowels are not irritated from a completely different condition; for example, an over- or under-active thyroid or parathyroid gland can cause bowel trouble, as can cancer.
Click the button bellow if you want to learn more about the anatomy of your gastro-intestinal system, so you can better understand your IBS.
Irritable Bowel Syndrome from allergies or "healthy" foods
Allergy Advice
MANY IBS issues are triggered when you eat certain foods. In some cases, you may have a food sensitivity; in other situations, IBS may be triggered by chemicals added to food (preservatives, flavorings, etc.). You may also experience IBS pain because of seasonal allergies cause your body to go into an inflamed state, making you more sensitive to foods you can handle during other times of the year. Here is my dietary advice.
To learn more if your foods, even foods you think are "healthy", may be the cause of your Irritable Bowel Syndrome!
Irritable Bowel Syndrome from an aging gut:
As you get older, your ability to produce hormones and digestive juices decrease. Pancreatic dysfunction results in low digestive juices, so your food doesn’t digest fully, irritating your digestive process. You can easily correct this by taking digestive enzymes (bio-chemical substances that help your body break down food) when you eat heavier meals. Oftentimes, if an elderly patient tells me their bowel movements are slowing down or if a young adult says they have severe constipation, I tell them to take digestive enzymes. It can make a world of difference.
Allopathic doctors are often so busy looking for disease that they forget that malnutrition can cause your symptoms. If you are low in magnesium or other minerals, the bowel muscles cannot function properly. Just like you can get cramps in your legs, you can get cramps in the smooth muscle that moves the fecal material through your intestines, leading to constipation. Similarly, the bowel muscles won’t work properly if you have too much of some minerals. If you are too high in calcium (eating too much cheese or taking too much calcium supplementation), you can experience constipation. Abnormal contractions of the intestinal smooth muscles can lead to diarrhea, constipation, or both.
A Poor Diet May Be Causing Your Irritable Bowel Syndrome Symptoms
I had a patient in her teens who had suffered from IBS since she was a toddler. Her bowels were so distended from having such severe constipation for more than a decade that her medical gastrointestinal specialists informed her parents that she needed to have her large intestine surgically removed and replaced with a colostomy bag!
During her first visit with me, I discovered every meal she ever ate consisted mostly of cheese and other dairy products. For example, typical meals for the day would be milk with breakfast, cheese pizza for lunch, and cheese tortellini for dinner. Her parents had spent tens of thousands of dollars on gastrointestinal specialists, and no one had ever asked about her diet!
I had her eat a cheese-free diet for a month and take digestive enzymes to help speed up the digestive process. The next time she saw me, she was having regular bowel movements. Years later, she is a healthy young adult.
Imagine! She almost had her colon removed!
Crazy!
And she is not the only case like this. Sadly, I have had several patients who were hospitalized multiple times a year because of their symptoms, only to be sent home with medical doctors claiming there was nothing wrong with them.
Just because the medical doctors didn’t understand the reason for the patient’s symptoms doesn’t mean there was nothing wrong!
Hidden additives in your food may be the cause of your Irritable Bowel Syndrome!
Avoiding foods with preservatives and artificial flavorings may help your IBS symptoms. In my case, I thought meat was a trigger. Then found out it was not the meat, but the hormones and antibiotics injected into the animals that I was reacting to!
If you want to learn more about how hormones and antibiotics in our meat can cause IBS, Click the button below:
Your Spine May Be Causing Your Irritable Bowel Syndrome Symptoms
Allopathic doctors are well versed in organic diagnosis (looking for diseases of the body’s systems), but they aren’t quite as familiar with nutrition or musculoskeletal conditions, which often mimic the symptoms resulting from problems with internal organs. Sometimes this results in a doctor misdiagnosing a musculoskeletal complaint as an organic complaint.
An example of this: I had a patient who was suffering from abdominal pain. He was diagnosed by his medical doctor with irritable bowel syndrome. The doctor prescribed an antispasmodic medication, but it wasn’t helping. Friends told him to talk with me to see what I thought.
Within five minutes of taking his history, I knew he did not have IBS. He had never had diarrhea or constipation until he started taking the antispasmodic medication. His only complaint was abdominal pain in the upper right quadrant (the right side of his body just below the ribcage).
Upon palpation, I determined that he simply had a rib out of alignment, which was irritating the joint in the front of the rib (the costochondral joint) and causing what seemed to be “abdominal pain.” A simple adjustment relieved him of his pain, and he was able to stop taking the medication (with his doctor’s approval) because not only was it not helping, but it was irritating his bowels.
I had another example of this when I treated a patient who had several attacks of abdominal pain a year. It was so bad that he would end up in the emergency room. Every time he went to the ER, the doctors couldn’t find the cause of his pain and would send him home with pain medication. When he heard about me, he came to see me instead of going to the ER the next time he had another episode of abdominal pain. I found that the thoracolumbar region of his spine was misaligned, causing pain to radiate (travel) into his abdominal region. One adjustment to his spine and his abdominal pain resolved. Now when he has an attack, he gets an adjustment instead of going to the emergency room, which not only saves him a ton of money, but also fixes the problem. It hasn’t failed him to date, and his abdominal pain is getting less frequent because I am teaching him how to strengthen and stretch to help stabilize his rib joints.
I can’t stress enough how important it is to get to the root cause of your symptoms so you can determine the appropriate treatment. If you have abdominal pain, don’t just look at the abdomen! Your symptoms may be a dis-ease of your GI tract or something completely different.
This is why you should have a team of medical professionals who can determine the true cause of your symptoms and then work with you to get you back to good health and help you maintain it.
You don't have suffer with IBS. Why wait?
If, after ruling out all of the conditions and causes I’ve described in this site, you are left with the diagnosis of IBS, then you are suffering from constipation, diarrhea, or both. The following chapters discuss your anatomy, so you can better understand your IBS and the effects of constipation and diarrhea.
CONSTIPATION CAN LEAD TO IBS and leaky gut syndrome. But before I explain the connection, you need to understand what constitutes constipation.
I would diagnose you with having constipation if you are not having a bowel movement at least once a day. You have healthy bowels if you are having a bowel movement two to four times a day.
The longer you go without having a bowel movement, the longer the waste products sit in your intestines, potentially irritating the lining of your intestines.
Understanding What Constipation Is
Think of your body as basically a tube. The outside skin is thick and tough, made up of multiple layers of cells; the skin’s top layers consists of squamous, keratinized, flattened protective cells. Some absorption is possible, but mostly these cells form a protective layer against the elements in which we live. Inversely, the tube’s inside lining is made of a delicate form of “skin” designed to let nutrients in and some of the waste out.
The intestinal lining is only one cell thick! The lining absorbs nutrients, and each cell increases the surface area for better absorption. However, when fecal material sits against it (if you are constipated), the lining eventually becomes inflamed.
Leaky Gut Syndrome
When the lining cells inflame, they activate the immune system. They also swell, causing the lining to stretch. When this happens, the toxic material can leak from the feces into the bloodstream. This is a case of true toxic waste literally poisoning you and leading to all kinds of health complaints (hence the diagnosis “leaky-gut syndrome”).
The stagnant fecal material can confuse the immune system, causing it to attack the body’s healthy cells. The body loses its ability to recognize self from non-self, resulting in autoimmune diseases. Autoimmune diseases can affect all parts of the body, including the skin (with eczema and psoriasis), the joints (with rheumatoid arthritis), and the nerves (with multiple sclerosis).
If the toxins overload the body’s ability to excrete them (when the kidneys can’t keep up) or neutralize them (when the liver can’t keep up), they are deposited in our tissues. The buildup of toxins causes aches and pains throughout the body, as in fibromyalgia.
In an attempt to sweep the problem under the carpet, the body hides the toxins in fat cells until our sewage system (the kidneys and liver) catches up. But if we never catch up, we hold on to those fat cells indefinitely, making it difficult to loose weight.
Constipation can also cause fatigue because the body needs a lot of energy to move the feces along, fight and/or neutralize the toxins that leak into the bloodstream, and feed the immune system, especially when the body may be malnourished because of a reduced ability to absorb nutrients.
So Should I Take a Laxative?
No! Do not take laxatives. Why? If you use laxatives on a regular basis, they won’t help in the long run. The medication only relieves the symptoms of constipation; it doesn’t solve the problem. The body will re-acclimate to expect the drug, and its effectiveness will diminish. Worse, if you stop taking it, a rebound effect may occur where you become even more constipated!
You don't have suffer with IBS. Why wait?
Combating Constipation
Constipation is uncomfortable, but you can treat it without resorting to laxative. Try the following suggestions individually or in various combinations:
· Drink plenty of water.
· Eat your fruits and veggies.
· Try Psyllium fiber, but with plenty of water. If you take Psyllium fiber and don’t drink enough water with it, the fiber can turn into a plug and bind you up further. More on this in Combat IBS Chapter 14.
· Massage your abdomen (as described in Combat IBS Chapter 22) and take your time on the toilet (as explained in Chapter 21). You might also try squatting when you’re constipated because that position is more efficient for having a bowel movement).
· Move and stretch your body (using the stretches and exercises in Combat IBS Chapters 24 and 25) to help wring the fecal material through the GI tract and out.
· Try doing a form of inversion to aid the parts of the intestine that normally have to work against gravity. (Combat IBS Chapter 25 has more information about inversions.)
· Relax and rest so your body can digest. (Combat IBS More on this in Chapter 21.)
Later on this webpage I will provide more information about the above points, as well as describe other helpful treatments to manage irritable bowel symptoms.
But before we get into that, let’s look at another pleasant topic…diarrhea.
WHEREAS CONSTIPATION can cause IBS, diarrhea is often a symptom of IBS.
If the intestinal lining gets too inflamed, it may stop absorbing nutrients altogether and just purge. Cases can be so severe that the lining expels its inflammatory, mucous-y waste along with the fecal material (as in pseudomembranous colitis).
What about doing a cleanse?
FOR MORE TIPS FOR CONSTIPATION
Treating Diarrhea
Diarrhea is no fun, and when it starts, you want to stop it as soon as possible. Thankfully, you can treat diarrhea several ways.
It may seem strange to you, but Psyllium fiber can help. Most people think fiber is used to treat constipation. However, Psyllium fiber is soluble, so it can sponge up the runny fecal material (again with plenty of water). If you don’t drink enough water, the Psyllium fiber can solidify and act like a plug, causing constipation. You don’t want to go from one extreme to the other. (More on this in Combat IBS Chapter 14.)
Diarrhea often causes the lining of the GI tract to become inflamed as digestive juices make their way into regions that can’t tolerate it. For example, the stomach can handle the acid it produces, but the esophagus and rest of the GI can’t. Using aloe vera soothes the lining of the GI tract. Just like when you apply aloe vera gel to soothe a sunburn on your skin, ingestible aloe vera gel helps soothe the “burned” lining of your GI tract.
When digestive juices go up into the esophagus or if it makes it too far down the intestines, the juices burn the sensitive thin skin lining these areas of the GI tract. Drinking an ounce of aloe vera daily while symptomatic helps coat and soothe the lining, helping it heal faster than it would on its own. Healing the lining of the GI tract may help resolve your diarrhea. (More on this in Combat IBS Chapter 15.)
You can take probiotics to help rebalance, if not restore, the good bacteria in the gut. If you take probiotics, make sure the supplement contains more than just acidophilus. We need a variety of bugs in our gut, and acidophilus is the least likely bug for you to be deficient in because it is found in dairy products like yogurt. (More on this in Combat IBS Chapter 10.)
Certain herbs may also help. A health practitioner can advise you on which ones are suitable for your specific needs. (More on this in Combat IBSChapter 16.)
Finally, stress can lead to diarrhea. Find ways to relax, and you may resolve your diarrhea. (More on this later - a.k.a. in Combat IBS Chapter 21.)
You don't have suffer with IBS. Why wait?
Should I Take an Over-the-Counter (OTC) Remedy for Diarrhea?
No! Medicines for diarrhea control the symptom but don’t cure the cause. Using medication over time limits its effectiveness, so if you find yourself in an acute situation where you need such a drug to work, it won’t work as well. Plus, most OTC medications have inactive ingredients that can cause allergic responses and make your condition worse. (More on this in Combat IBS Chapter 8.)
The best way to treat your diarrhea is through diet, soluble fiber, plenty of water, and de-stressing.
To see Dr. Karin's anti-diarrhea recipe, check out her Facebook Live:
Remember, a happy GI tract makes for a happy immune system, and a happy immune system makes for a healthy body. A healthy body makes for a happier mind, and a happier mind calms the nervous system so you can rest and digest, which makes for a happier GI tract. Supporting the health of your GI tract and spine should help your IBS, whereas medications can make your IBS worse.
STRESS can be a cause of your IBS:
SUPPLEMENTS CAN HELP WITH IBS:
Insomnia can affect IBS
You need to rest to digest. The following is our tips for insomnia:
We have advise for GERD, acid reflux and
or a spastic gall bladder:
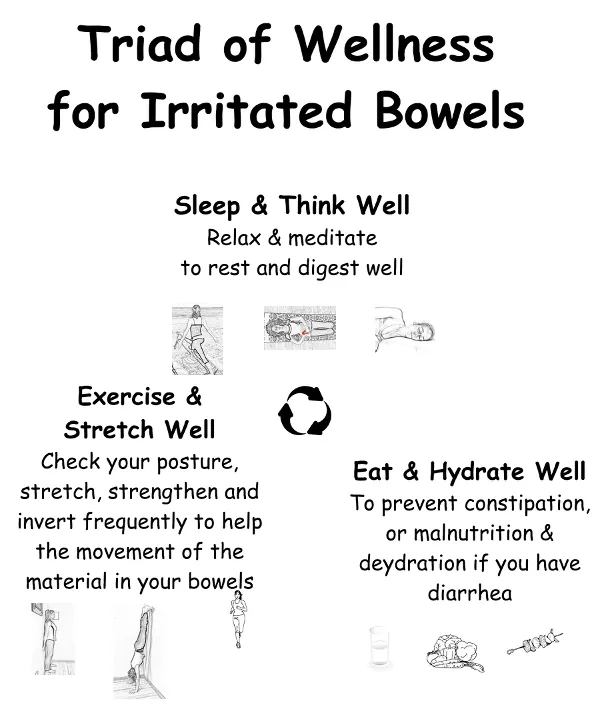
In conclusion, to improve Irritable Bowel Symptoms,
you need to eat well, sleep well and move well.
Find a health care practitioner to help you determine what this means for your bodies specific needs.
To learn more about IBS, check out my book: Combat Irritable Bowels.
To learn more about how we treat here at Drummond Chiropractic, CLICK HERE.
To go back to our home page, CLICK HERE.
You don't have suffer with IBS. Why wait?
Drummond Chiropractic, LLC
More than chiropractors, we are wellness experts.
We can help you with your Irritable Bowel Syndrome!
565 N Walnut St
Bloomington, IN 47404
(812) 336 - 2423