The most common cause for heel pain is plantar fasciitis. Plantar means bottom of the foot and fascia is a type of strong, fibrous tissue. Plantar fasciitis means inflammation of the ligament/facial tissue that runs along the bottom surface of the foot, helping to hold up the arch, which originates from the heel bone, where it is often most painful. Treating plantar fasciitis may involve a combination of taping up the arch for support, anti-inflammatory drugs, arch supports or orthotics, stretching, Graston and rehabilitative therapy.
PLANTAR FASCIITIS
Plantar fasciitis occurs when the tissue that connects the heel to the toes becomes inflamed. This inflammation causes pain on the bottom of the heel that can continue to grow in intensity over time.
Risk factors include:
- Flat feet
- High arches
- Non-supportive shoes
- Inappropriate shoes (too small)
- High Heels
- Obesity
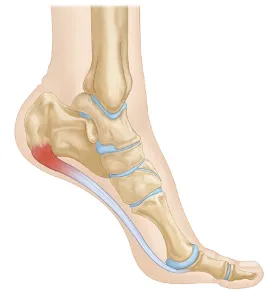
Figure 5‑1: The plantar fascia.
COLLAPSED ARCHES strain the plantar fascia (the tissue on the bottom of the foot) more than any other tissue in the feet because the plantar fascia stretches every time the arches collapse. This causes every step to irritate this tissue, which can lead to inflammation and pain. |
Plantar fasciitis is inflammation of the plantar fascia. Like any inflamed tissue, it is very tender when moved. It’s like having tennis elbow of the foot. However, unlike the elbow, the foot is weight bearing, so just standing irritates the tissue.
To make matters worse, the plantar fascia is the most distal tissue of the body; it is the furthest tissues to supply blood to and drain waste from. Marry this with the fact that the plantar fascia is squished when you bear weight on the foot, and you can understand why this is such a painful condition!
Because we rely on our feet so much, it is difficult to treat and recover from plantar fasciitis.
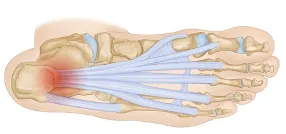
Figure 5‑2: Heel pain can be caused by inflamed tissue anchored to it.
Every time your foot hits the ground, the weight of your body compresses the tissues in the heel, squishing out the needed nutrients. Plus, the momentum of the movement causes the arch to strain or sprain. With every step, the ligaments and tendons pull on the bones they are anchored to. This is why people develop more pain with walking (unlike other conditions that are alleviated by walking).
Eventually, walking can inflame the tendons and ligaments to the point that your feet hurt all the time, not just when you walk.
If the foot remains swollen with inflammatory proteins, often the first step is very painful (just like other conditions) and worsens with every step (unlike other conditions).
Treating Plantar Fasciitis
If you suffer from plantar fasciitis, you can recover, but treatment is necessary.
See a healthcare provider to confirm that you have plantar fasciitis. If you do, you need to support the plantar fascia with orthotics. (See Chapter 3 for more about orthotics.)

Figure 5‑3: Orthotics help plantar fasciitis.

Home care includes heating the calf muscles for five to ten minutes, stretching the lower leg and foot as described in Chapter 19 and then massaging the area of foot that is in pain with ice for two minutes, as described in Chapter 20.
Avoid any activities that cause or aggravate your foot pain.
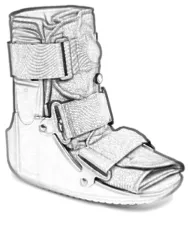
Extreme cases may require the use of a boot to keep the weight off of the plantar fascia. If you need to wear a boot, make sure to put an orthotic in it because boots are typically flat. The lack of arch support can worsen the plantar fasciitis.
Make sure you find a shoe to wear on your asymptomatic foot that has a higher sole so your leg lengths remain the same. You don’t want to mess up your back while trying to heal your plantar fasciitis!
More on Treating Plantar Fasciitis:
Again, there are many conservative treatment options for plantar fasciitis, including a stretching regimen, icing, footwear modifications, anti inflammatory medications and weight reduction to lessen impact on the feet.
More severe cases may be treated with additional padding and orthotic devices, the use of a walking cast, night splints and physical therapy. Surgery to detach the plantar fascia is an option, but only if all other treatments have been ineffective.
If you are experiencing heel pain, schedule an appointment with us today. The sooner you get treatment, the sooner you can walk without pain. With three experienced chiropractors on staff, we should be able to schedule in today. Click Here to schedule with us and start your journey to pain free feet.
If we determine that we CAN help your condition, we will treat same day, demonstrate home exercises and stretches you can do to speed your recovery. We will follow up the appointment with a Report of Findings email that details what your condition is, what our treatment plan is and lists the prescribed exercises and stretches, complete with videos that you can follow along with. To learn more, check out:
You don't have to be in pain. Why wait?

to schedule with us.
We offer FREE foot scans.
SITTING AND FOOT PAIN THAT MIMICS PLANTAR FASCIITIS
At a minimum, prolonged sitting increases swelling of the legs, and over time, the swelling can become uncomfortable and even painful.
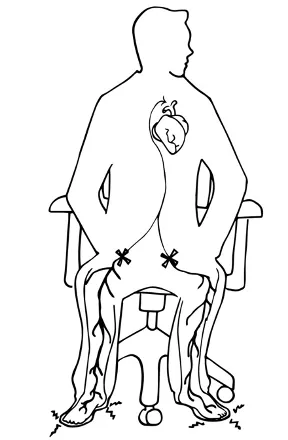
Figure 14‑1: Prolonged sitting can cause foot pain.
I have had patients come to me thinking they have plantar fasciitis because they feel severe foot pain when they first stand up. Upon questioning, I discover that their pain improves with walking. This tells me they don’t have plantar fasciitis, but likely are experiencing pain caused by swollen lower extremities.
When your feet are swollen, it hurts to bear weight at first. As you move around, the fluids causing the swelling drain, and the pain lessens. It doesn’t take a noticeable amount of swelling to be painful. Patients who have swelling caused by too much sitting are often relieved to find out they don’t need to buy expensive orthotics.
You don't have to be in pain. Why wait?
to schedule with us.
Other Causes of Swollen Feet
Feet can also swell from standing for long periods of time on a regular basis, flying in airplanes, long commutes (sitting too long without moving), genetic weakness of the valves of the blood and lymph vessels that allows back-flow of fluid, or damaged vessels.
Back-flow in the veins and/or lymph vessels puts even more pressure on valves and causes them to stretch apart, allowing even more back flow. Like a balloon, once the valves have been stretched, it’s easier for them to stretch again, making the valves less able to hold back further back-flow.
To relieve pain from weak valves, you can perform the Foot ABCs for Lymphatic Drainage (described in Chapter 19) and elevate your feet often. This drains the lower extremities of the excess fluid.

Figure 14‑2: Lymphatic drainage.
If the valves are damaged enough, the relief will be temporary because standing up will cause the legs to swell again.
If raising the feet above the heart is not enough to provide lasting relief, you may need to wear compression stockings. You can choose from a variety of compression hose that come in different lengths and amounts of pressure.
Graduated compression socks are effective at preventing and treating varicose veins and swelling of the lower extremities. They gently squeeze the vein and lymph vessel walls together so they can close and prevent the back-flow from occurring.
Usually medical compression stockings are 15 mmHg or higher to compress the legs enough to support the veins and lymph vessels of the lower legs. To learn more about the lymphatic system and how to drain it, click below:
Self massage and mobilization techniques for the foot
EXERCISES AND STRETCHES FOR FOOT PAIN
THE ABOVE IS FROM DR.KARIN'S COMBAT FOOT PAIN. Specifically, Chapter 19. Here we explain how to strengthen the muscles of the lower extremities to help support the foot and stretch the muscles and joints of the lower legs and feet to help alleviate foot pain. You don't have to be in pain.Why wait? CLICK HERE to schedule with us. |
CLICK HERE FOR MORE CONDITIONS WE TREAT
TO BE WELL YOU NEED TO
MOVE WELL, SLEEP WELL AND EAT WELL
Want to see what else we would advise for you?
Why wait?
Drummond Chiropractic, LLC
Plantar Fasciitis Specialists
Podiatry Chiropractor Specialist
565 N Walnut St
Bloomington, IN 47404
(812) 336 - 2423







