One moment everything may seem fine, when suddenly you’re involved in a serious collision. Most people have one thing on their mind after a car accident is their car! However, it’s important to remember that you and your injuries come first. A visit to a chiropractor should always follow an auto injury, as chiropractors are specialists in damage to soft, tissue, joints, nerves and more.
Are you looking to fully recover from your auto accident
as quickly as possible?
You don't have to be in pain!
We can help!
How Can a Chiropractor Help Me After My Auto Accident?
Chiropractors are able to treat neck and back injuries associated with auto accidents. But here at Drummond Chiropractic, we have experienced injury experts. Dr. McCoy is a sport injury specialist, so is well trained in treating injuries. Dr. Karin's personal experience with Whiplash resulted in her publishing her journal of her healing process. In "Whiplash to Wellness" (pictured above), Dr. Karin details her whiplash symptoms, whiplash treatments, explanation of whiplash and so much more. Click here to check it out on Amazon.
You don't have suffer. Why wait?
After an auto accident, some individuals experience indicators of whiplash injuries right away, such as blurred vision, headaches, shoulder pain, dizziness, reduced range of motion and arm pain. Whiplash can also result in minor back injuries, muscle injuries, ligament problems, and disc damage. Other individuals may be injured and feel nothing at all.
Treating pain or whiplash should never be secondary to bringing your car at the mechanic or working with your insurance company. If you’ve had an auto accident recently, your first priority should be taking the initiative to visit your chiropractor!

We are ACE Chiropractors: Affordable, Convenient and Effective.
Why Wait? Get out of pain TODAY!
You don't have suffer. Why wait?
The following is an excerpt from Dr. Karin Drummond's "Whiplash to Wellness: book.
IT HAD BEEN A LONG HARSH WINTER, and for the first time in a long time, the sun popped out from behind the clouds on an afternoon that I had off work. It felt so good to feel the sun’s warmth, effectively thawing out my bones. I had company over for a late lunch, and we ate out on the deck.
Then my cell phone rang. A patient, P.A., was on the other end. He was in dire pain, suffering terribly with severe, acute neck pain. I knew he wouldn’t have asked me to treat him during my off hours unless it was really bad. He had already been to the ER. Sadly, the muscle relaxers the doctor there gave him just made him feel loopy; they weren’t helping his pain or range of motion. He had to be able to go to work.
How could I say no? Of course I would go to my office to help him, despite the beautiful day. So I told him I would see him, if he didn’t mind seeing me in my street clothes. He didn’t care. He was just happy that I would work on him.
He walked into the office not being able to move his neck and wearing an expression of torture. As expected, he left with an expression of relief and the ability to turn his head again.
I really do love my job.
I sat down to finish up some paperwork. My husband, Dallas, texted me to remind me to get the mail out of the mailbox before coming home.
It was shortly after 6 p.m., so I decided to get going. We were planning on going to a comedy show with friends, and I wanted to shower and change before going to the show.
I pulled out of the office’s parking lot, turned left (west), and went into the far right lane.
A bus was ahead of me, in the middle lane, slowing down to turn left. Unbeknownst to me, another vehicle, hidden by the bus, was heading east toward me.
There I was, driving straight in clear weather conditions, with nothing in front of me, when suddenly, a vehicle came out of nowhere and entered the intersection right in front of me. My instincts took over, and I slammed on the brakes, despite having no time to stop. I T-boned the other vehicle hard.
I was going at least 40 mph at the time of impact. My little Toyota Corolla hit the other driver’s Jeep Cherokee so hard that it spun the SUV more than 180 degrees, and her back tire on the driver’s side blew out when it hit the curb.
With my body’s forward momentum and my car going from 40 mph to zero in less than a second, my buttocks left the seat. My seat belt pressed hard against my chest, stopping me from hitting the steering wheel. I continued to brace, gripping the steering wheel intensely, expecting the airbag to deploy. I slammed back into my seat. The airbag never deployed.
My first thought was, I must not have hit her as hard as I thought I would, or else the airbag would have deployed.
I was dazed but didn’t feel hurt. I closed my eyes and did a quick assessment. No bones felt broken. I could move all of my joints without pain. I opened my eyes. I didn’t even see a scratch on my skin. On a scale of 0 to 10, my pain was at zero.
Again, I felt lucky that the airbag didn’t deploy. If it had, it would have injured my face or, worse, broken a rib. It would be impossible to work with a broken rib. I couldn’t afford not to work. Not only did I have bills to pay, but I had patients who needed me.
I called my husband to let him know that I had been in a motor vehicle collision. It wasn’t my fault, I told him; I just couldn’t stop in time.
He took this to mean that I had been in a minor fender bender. He reminded me to get the other driver’s information (name, driver’s license, license plate number, insurance information) and take tons of pictures after calling the police.
I called 911 to inform them of the situation. I also called my insurance agent from Indiana Farm Bureau to see if he had any advice. He asked if I was OK and then offered to come over (he wasn’t too far from the site of the crash) to make sure everything was handled correctly.
This is why I advise people to get insurance through a company that has a local agent who can be your personal advocate. I’ve had to have my agent come out and help us with insurance claims and work as our advocate many times over the years, and having a local agent has been invaluable.
My agent even offered to give me a ride home. I agreed, totally forgetting my plans for the evening.
After hanging up with him, I finally got out of the car. The other driver got out and asked if I was OK. I replied that I currently felt fine, but I treat people who have experienced collisions like this all the time, and I would likely be sore in the morning. I didn’t think much of it because my husband is a great chiropractor, and I had handled other injuries without any problems.
The other driver and I exchanged information while waiting for the police to arrive.
The emergency response crew arrived first. They blocked traffic to clean up the glass and oil.
I then started taking pictures of my car. Everything seemed surreal. I was surprised to see that the front of my car looked like an accordion. The hood of my car was squished in half.
The police arrived. An officer asked both of us to recount what had happened, and our stories matched. It was deemed that the collision was indeed 100 percent the other driver’s fault. The officer asked for my driver’s license and registration. I went to the passenger side of the car to get them, but the passenger side of the hood was crushed in so far that I couldn’t open the passenger door.
As I struggled to force the passenger door open, the EMT crew stopped me. One explained that the airbag should have deployed, and may yet deploy, which would injure me if it deployed while I was reaching for my items. They were going to disconnect the battery so I could gather my paperwork.
The damage to my car was so severe that they couldn’t disconnect the battery, so one of the EMTs went in with protective headgear to get my papers.
It was at that moment, strangely, that I realized the extent of the damage to my car.
I turned to the police officer and told him half-jokingly, “Now I am feeling shaken up by that bit of news.”
I must have looked unwell because he asked me to sit down, but not where we were standing because we were close to traffic. So I moved to the sidewalk, and despite feeling a little silly, I sat down.
I am glad I did because my body started to shake slightly and my hands began to tremble. This was a sure sign that I was getting over my adrenaline rush, so my blood pressure was likely dropping, which could result in fainting. Resting on my buttocks on the sidewalk would be less embarrassing than fainting in front of all the onlookers.
My husband called, asking what was taking so long. I said I had to wait for a ride home.
He was surprised because I had underplayed the seriousness of the crash. In my shock, I hadn’t realized during our earlier conversation that my car was too damaged to drive home. I texted him some of the pictures I took, and he immediately said he was heading over to pick me up.
This new driving arrangement made more sense because we had to go to the comedy show within the hour, and I no longer had time to go home first. I still had to wait for the tow truck to remove my car and for the police officer to give me his report.
I stood up as everyone finished the cleanup. My insurance agent showed up seconds before my husband did.
When my husband arrived and saw my car, he was even more surprised. Dallas, being a chiropractor as well, agreed with me that I was going to feel pain in the morning. He said he would treat me after the show that night.
My insurance agent, who had more than thirty years of helping people after collisions, said with an impact like that, I was likely going to be too sore to work the next day. My husband reminded him that I was the kind of woman who went to work the day after having babies, so I would be able to work through any pain this crash caused me, no problem.
I agreed because I was in denial about the severity of my injuries. I had too many patients scheduled the next day who needed their treatments. Plus, I thought I could still enjoy the comedy show and afterward go to a salsa dance downtown. I had been looking forward to this salsa party for weeks because a huge turnout was expected, with more than a hundred people who really knew how to salsa! How fun! Of course I was going to go. Remember, I’m a tough cookie.
Dallas took the rest of the items out of my car and put them in his SUV. He asked if I remembered to get the mail.
I had not.
He half-jokingly suggested that if I had picked up the mail like he had told me to, I wouldn’t have gotten in this crash. That’s what I get for not listening to him. LOL.
Amazing how little things like that can drastically change the outcome of one’s day.
MY CAR WAS TOWED AWAY, and off we went in Dallas’s car to join our friends. I was the center of attention before the show, explaining what had happened just moments earlier. After they saw pictures of the crash, no one could believe I had come to the show. I explained I would rather be laughing with friends than crying about the collision at home.
One of my friends who had experienced whiplash personally said I had just experienced a very traumatic event. She added that it was OK if I wanted to go home and take care of myself. I poo-pooed her suggestion and the show began.
I stretched in my chair throughout the show and even stood up several times to stretch. I knew that sitting still after a soft tissue injury like this was a bad idea. I knew it was important to keep moving to help prevent my joints from locking up.
I drank a couple of glasses of red wine to calm my nerves, and I made sure to drink plenty of water between sips of wine to stay hydrated to combat the wine’s dehydrating effects.
Surprisingly, within an hour of the show starting (within three hours of the impact) and despite my efforts to stay loose and hydrated, my neck and mid-back started to seize up. By 9 p.m. my neck was almost completely immobile and in moderate pain.
I told Dallas that I wasn’t sure if I could stay until the end of the show, which would be over by 9:30 p.m. He said to keep stretching and that we would head over to the office right after the show.
Another friend at our table, who also had suffered from whiplash, gave me some CryoDerm (a cooling gel with arnica and other herbs that help muscles heal).
Ironically, she had gotten it at my office to help with her flare-ups of pain from her motor vehicle collision. I applied it liberally to my tightening muscles.
Dallas and I ended up leaving before the show was over. I just couldn’t stand being in a seated position any longer.
I couldn’t believe I could go from no pain to such severe, immobilizing pain in such a short amount of time. I would have rated the pain a 10 out of 10! To give you an idea of how bad this pain was, I had home births and would have rated that pain a 4 out of 10 because I was able to talk and smile at jokes during that pain. This pain was indescribably sharp, intense, and persistent.
I have seen and studied delayed onset of symptoms (DOS), but honestly, I didn’t think a person could hurt so bad without having at least some pain at the time of injury. I thought I would wake up with mild pain the next morning, not have searing 10+ out of 10 pain within hours of the impact. I felt like I had a knife laced with acid in my back!
It was very humbling. Because I had regular adjustments and did yoga, I thought I was in such great shape that I was above such injury. I couldn’t even imagine how a person of poorer health would feel with the same type of injury. I started to understand why some of my patients simply needed to take pain-relieving medication.
You don't have suffer. Why wait?
Why Feeling Pain Is Delayed
You might be wondering, why it took so long for me to feel pain when the injury occurred hours earlier.
When our bodies experience pain or trauma, our prehistoric fight-or-flight system kicks in. Evolutionarily, it was an advantage not to feel pain immediately. In those days, when prehistoric humans were injured, they couldn’t afford to feel pain while the threat was still present. If they felt pain, they wouldn’t be able to fight or flee from the cause of the injury; then they would likely die and not pass on their genes.
We still experience the fight-or-flight reaction today. When we are severely injured, our brains release beta-endorphins, which are basically powerful opiates that block pain.
After a motor vehicle collision, the damage is there; you just can’t feel it. But over time, our kidneys filter these opiates out of our system, and we start to feel the effect of our injuries. Some people report pain three or four hours after the trauma; their injuries are so bad, they feel the pain as soon as the opiate levels start falling because it takes more opiates to block such severe pain. Other people may not feel any effects of the impact until the next day because it takes longer for the body to filter out the opiates to a level low enough to feel the pain.
If the pain starts two days after the trauma, then the person’s pain is likely because of their compensation mechanisms causing injury. For example, a driver feels right knee pain weeks after the car crash. This pain may be caused by the arch of the right foot having dropped from the impact of slamming on the brakes during the collision. This can cause knee pain weeks later because the body has changed its gait cycle to compensate for the collapse of the right arch with every step, which places stress on the knee.
|
BY THE TIME DALLAS AND I got to our office, my muscles were even more spastic. They were in such spasm that Dallas could only do passive therapy (gentle mobilization) because he couldn’t get my neck close to a position where he would be able to adjust it.
At this point, you may be wondering why I didn’t go to the hospital and get an X-ray.
X-rays are great for determining fractures, examining bone pathology, and showing evidence of instability and muscle spasm (Figure 3-1).
Dallas checked my spine with a 128-Hz tuning fork to see if it increased my pain (Figure 3-2). If it had, there was likely a fracture. This technique was used before X-rays, but I still find it useful. Sometimes a tuning fork will catch a hairline fracture that was missed on an X-ray.
Whiplash is often “Invisible”
According to studies, whiplash injuries often fail to show many abnormalities on an X-ray, even with severe or unstable lesions.[1] This is because the image of the neck is taken when the neck is not moving. Damage to ligaments and muscles affect how the neck moves, making it hypermobile and causing pain. X-rays don’t usually reveal how an injured neck looks at rest. If you get an X-ray after a car crash, ask about getting an X-ray taken with your neck in flexion (bending your head forward) and extension (bending your head back). With these images, a healthcare provider is more likely to see any instability caused by a motor vehicle collision. If these images still fail to show any signs of injury, your healthcare provider may order more specialized imaging like Dynamic Motion Imaging that uses fluoroscopy (like an X-ray video of your neck moving).
Many argue that you should X-ray after any trauma. If the instability is extensive enough, a chiropractor can harm someone severely with a manipulation. There have been cases of unknown bone pathology before a trauma that would not have been detected without X-ray. I have heard of people walking into a clinic with a broken cervical spine (not something you want to manipulate at all).
If in any doubt after a motor vehicle collision, you need to get imaging!
But I am not a typical patient. I am a chiropractor, and I can feel my symptoms. I didn’t need an X-ray to know I had a bad case of whiplash. I wasn’t thinking about litigation at that stage. I just wanted my chiropractic husband to work on me so I could start getting better. The last thing I wanted to do was go to a hospital so late at night to get imaging I didn’t need to get well.
After looking at all the evidence, Dallas adjusted my mid-back, but he left my neck alone. My neck was just too sore to touch or examine, let alone manipulate. He had to adjust my mid-back in a standing position because lying on my stomach was impossible. It was just too painful to sit or lay down.
The adjustment gave me some relief, but I was mortified to realize that I was going to miss the salsa party that night. I could not sit or lie down without pain, let alone dance.
Mortifying!
Why Does Whiplash Hurt So Bad?
It makes sense that a broken bone hurts. You see a hard structure with a break in it. You see the cast that needs to be worn. For us visual creatures, it makes sense that a fractured bones hurts—a lot—and hurts as soon as it is broken.
When I look at pictures of myself taken within two days of the car crash, I can see why people didn’t realize how hurt I was. You can’t see how I couldn’t move without searing pain because I wasn’t moving.
I simply couldn’t turn my head because my protective muscles wouldn’t let me. But just standing there, I looked great. So the pain couldn’t be that bad, right?
I can’t state strongly enough how much pain I was in when this picture was taken. There is just no way to describe the pain that does it justice. But why? Why is there so much pain in the neck and/or spine?
Basic Spine Anatomy
At risk of oversimplifying, the spine is made up of a column of bones with intricate connections. The bones are lined with fascia, ligaments, tendons, and muscles (both big and small). The neck and low back have lordotic curves, and the middle back has a kyphotic curve.
The neck and low back are more vulnerable to rear-end collisions, and the middle back is more vulnerable to front-end collisions.
So How Does the Whiplash Injury Occur?
Without getting complicated, I’m going to use a balloon analogy. When you first try to blow up a balloon, it’s really hard to inflate it. If you stretch it first, it’s easier to blow up. If you deflate it and blow into it again, it inflates even easier.
This is similar to what happens in a whiplash injury.
Imagine two bones surrounded by a thick rubber balloon holding the bones together. If you stretch the bones apart with some pressure, they return to their normal tight position when you let go. But if you use enough force to overstretch the bones apart, the rubber stretches to a point where it thins out. When you let go of the bones, they won’t be held together as tightly as before.
The “balloon” has been “blown up”, overtly stretching it. Now it doesn’t take as much force to “inflate” it.
You are now vulnerable to injury with less force than before the car crash! By simply leaning forward to reach for something, the bones may move apart abnormally and painfully, and bam—you feel severe pain as the bones shear apart.
Before the advent of videography that could capture one thousand frames per second, the scientific explanation of whiplash was that it is simply a hyperflexion/extension (head whipping back and forth) injury (Figures below).
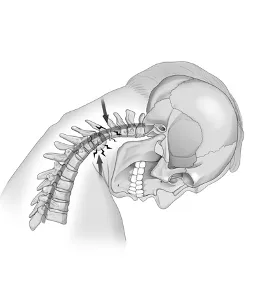
Other experts would argue that the neck could handle such movement without injury, so whiplash was “faked” by people who were just looking to get more money out of the litigation process.
Since the late 1990s, with the ability to see what happens in the first 200 milliseconds of a deceleration injury, we have learned that damage occurs even before the head whips back and forth! At impact, damaging forces cause the vertebrae in the neck to slip forward in an unnatural way, causing injury (Figure 4-3). Using my earlier analogy, this is what “overtly stretches the balloon.” Then, without having a “tight balloon” holding the bones together, when the head does whip back and forth, further damage occurs!
So the other experts were right: A healthy, undamaged neck can handle a whipping back-and-forth action, but it can’t handle that motion after the neck’s supporting ligaments are damaged in the first 200 milliseconds.
You don't have suffer. Why wait?
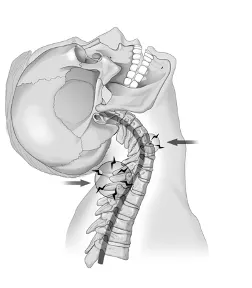
Mechanism of whiplash from being rear-ended
The injury caused by being rear-ended occurs even before your head whips back and hits the headrest. When a vehicle is hit from the rear, the bones in the lower neck slide forward and stretch too far apart in the first 200 milliseconds.
At impact, the lower neck bones are jerked forward with the body before the upper neck and head even move. This can cause injury in less than one-hundredth of a millisecond after the impact.[1]
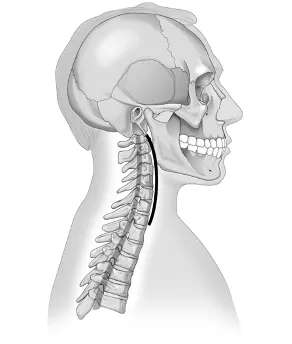
This shearing force causes the normally lordotic C-curved cervical spine (the normal anatomy of a neck) to misshape into an S-shaped cervical spine
In the images above: The dark lines depict the change of the curvature in the neck from a neutral C curvature to an aberrant S curvature in the first 200 milliseconds after impact.
Even though the shearing movement only takes milliseconds, it can cause so much abnormal movement to the middle bones of the neck (C3–C5) that it can injure the phrenic nucleus.[1] The phrenic nucleus is the “house” of the nerves that supply the diaphragm so we can breathe without having to think about it. Damage to the phrenic nucleus can result in everything from hiccups to affecting one’s ability to breathe. Poetically put, “Nerves C3, 4, and 5 keep the diaphragm alive.”
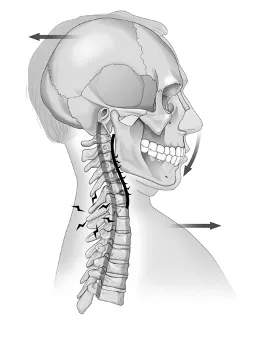
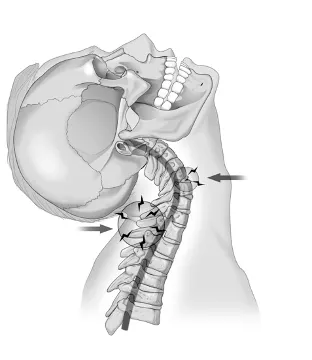
Just 200 milliseconds after impact, the head and the upper neck whip back into extension while the torso is restrained by the seat belt. The figure above shows the hyperextension to an already injured neck leading to disc herniations and possible fractures. This is where hyperextension injuries occur. When the neck jerks back into hyperextension, the deeper posterior structures are crushed as the bones slam together. Without the support of their ligaments, the vertebrae can slip out of their normal position and squish the tissue between them. If the head jerks back far enough, muscles and ligaments in the front of the neck can sprain, tear, and bleed. This can result in one or more blood clots in the soft tissue (which can also elicit pain).
The deeper structures of the front of the neck can get hyper-stretched as well. The anterior longitudinal ligament (the ligament that supports the front of the vertebrae) can tear, leading to instability of the neck bones; the anterior annular part of the discs can tear; and the endplates of the vertebral bodies can fracture.[2]
Then you have the rebound effect.
After all the shearing and hyperextension injuries, the body is thrown forward into hyperflexion (Figure 4-6), where the injured discs are now squished and twisted. This creates a perfect condition for the jelly material inside of the discs to rupture out.
Mechanism of whiplash from a front-impact collision
With a front impact (like mine), the forward momentum of the upper body causes a shearing action to the discs of the middle (the kyphotic thoracic) spine.
At impact, the mid-back to low-back bones are jerked back before the upper back bones even move.
So, with a front impact, the top vertebrae slide forward on the vertebrae below it (Figure 4-7). Facet joints help limit this type of movement, but if the force is strong enough, it can crack the cartilage and/or fracture the bones of these joints.
Plus, you still have loading (compression) forces on the spine. These forces occur when the body slams down into the seat after being launched off the seat on impact. The discs in the spine can bulge, if not rupture, when the body drops back into the seat.
The spine may also experience twisting forces as the body is pinned back on one side with a seat belt (Figure 4-9). The twisting forces result in some of the facet joints crashing together and other facet joints being torn apart. Both actions can result in injury and pain.
These forces can rupture (herniate) the discs as the vertebrae compress. The compression squishes the jelly material out from the center against the discs’ strained outer fibers, which are twisted more than they can handle. This creates a perfect condition for the jelly material to rupture out of the disc.
The rebound effect in a front-end impact throws the body back. If the impact is hard enough, the neck can be subjected to shearing forces similar to those that occur in a read-end collision.
If intense enough, a deceleration injury can be life threatening. Hyperextension can tear the wall of the large artery coming out of your heart (aortic disruption). Hyperflexion can compress your heart enough to bruise it or fracture your sternum and/or ribs without even hitting the dashboard or steering wheel.[1]
Of course, bones can break if there is a direct impact.
Can a Person Be Injured or get whiplash When There Isn’t Much Damage to the Car?
Yes! I can’t tell you how many times I have heard from my patients that the insurance company for the at-fault driver is claiming the driver or passengers in the other vehicle can’t be seriously injured because there wasn’t much damage to the vehicle.
This is simply not true! These insurance companies are trying to get out of paying for something they are responsible for. I have witnessed too many instances of insurance companies trying to strong-arm my patients into thinking their case is weak and their symptoms are exaggerated. Insurance companies save a ton of money by getting people to settle their cases too early, which results in patients not getting the care they need to fully recover.
I am writing this book to give you and/or your loved ones the backing you need to get a fair settlement. If you’re in pain, you are not well. Don’t let insurance companies convince you that you don’t have a case. Find the treatments that work for you and continue your care until you are well! Don’t settle for less.
You can suffer injuries inside a car that doesn’t show much damage, especially an older car. Newer cars are designed to crumple on impact, which absorbs the force of the collision. When you’re in a crash in a newer car, the metal bends on impact instead of your body getting jolted or thrown around inside the car.
Older cars have thicker steel. During an impact, the steel doesn’t give as much, so the force transmits to the people inside the car. If the cars collide at stiff points (like the trailer hitch), the car may not have much damage, but the passengers will be injured from the jostling force of the impact.
You don't have suffer. Why wait?
What Speed Does It Take to Get Whiplash?
You can get whiplash at speeds much lower than those involved in a motor vehicle collision. I have had patients who have suffered a whiplash injury after they’ve slipped on ice, jarring their body and causing their head to whip back in an unnatural position, resulting in further injury.
Speed is just one factor that determines how severe an injury will be. If the angles of the shear forces on the body are such that they reinjure an old injury or cause a new injury, pain results.
Now that you understand a little bit about how physical damage to the body occurs, let me explain why relatively small muscle strains and ligament sprains hurt so bad.
Understanding How Our Bodies Communicate Pain
When we experience a car crash, our muscles kick in and hold us together, since the ligaments that hold the bones of our spine in alignment are now too stretched and loosened too. Adrenaline courses through our body, so we don’t necessarily feel the pain right away. But as the adrenaline wears off and the muscles start getting tired from holding the bones together in a way that they’re not designed to, bones start slipping out of their regular position, putting pressure on our nerves. These nerves have a direct link to the brain. I call this “core pain.”
When the spine is injured, or a neck suffers with whiplash, the nerves going into and out of the spine can be affected. If the cluster of nerve cells known as the dorsal root ganglion is injured, the body’s distal nerve pain signals to the spinal cord are amplified, increasing the sensation of pain. This pain originates close to the spine with a direct connection to the brain. This pain is difficult to block.
When your extremities are injured, two nerves transmit information to the brain: (1) A sensory nerve goes from a distal region of the body, like an arm, hand, leg, or foot, to the spine. (2) A post-synaptic nerve cell continues the transition of information up the spine to the brain. Between these two nerves, the pain response delivered to the brain can diminish or increase.
The space between nerves is called a synapse, which is where chemicals (neurotransmitters) exchange information from one nerve to another. Synapses can be affected by chemicals from surrounding nerves that can deaden the pain. When you experience distal pain, pain gates can close, diminishing the pain. This is why rubbing the area makes you feel better; the touch receptors close the pain gates so the brain can sense their touch input.
Synapses can also be affected by chemicals in the blood, like adrenaline and pain-relieving drugs. Distal pain, like knee pain, is easier to block with pain-relieving medicine than core pain, like spinal injuries.
Nerves inside the spine have a direct link to the brain. This type of pain cannot be blocked, short of medical anesthetics. Spinal injuries cause deep, intense, crippling pain. The pain is compounded by the exhausted muscles still trying to hold things together, producing an increase in metabolic waste as a side effect. Metabolic waste is neurotoxic, which also increases the sensation of pain.
The chronic contractions of a spastic muscle constrict the blood vessels that bring the muscle the nutrients it needs to function and heal. The contractions also constrict the veins and lymphatic vessels, preventing the drainage of toxic metabolic waste.
This buildup of metabolic waste surrounding the muscles and nerves irritates them, making the muscles tender to touch and causing the nerves to fire even more pain signals to the brain. Then the muscles attempt to spasm more, trying to stabilize the injury even further.
To learn more, check out Dr. Karin Drummond's book, "Whiplash to Wellness"
Or better yet, call us.
You do not have to be in pain!
We can help!
[1] Swan, Swan, and Swan, “Decelerational Thoracic Injury,” Journal of Trauma, Injury, Infection and Critical Care.
[1] Yoganandan et al., “Whiplash Injury Determination,” Spine.
[2] Davis et al., “Cervical Spine Hyperextension Injuries,” Radiology.
[1] Davies, “C3, 4, 5 Keeps the Diaphragm Alive,” American Journal of Forensic Medicine and Pathology.
[1] Gentle, Golinski, and Heitplatz, “Computational Studies of ‘Whiplash’ Injuries,” Proceedings of the Institution of Mechanical Engineers.
Drummond Chiropractic, LLC
565 N Walnut St
Bloomington, IN 47404
(812) 336 - 2423